When Your Child Has Nosebleeds
Nosebleeds (epistaxis) are common in children. They rarely mean a serious problem. Nosebleeds in the front part of the nose are the more common in young children and usually easy to stop. Bleeding usually occurs in a single nostril only. A newborn baby with nosebleeds may need to see an ear, nose, and throat (ENT) specialist.
Nosebleeds in the back part of the nose, near the throat, are less common in children than nosebleeds in the front. A nosebleed that occurs deeper in the nose often comes out of both nostrils. It's harder to stop. These can be more serious and cause a lot of blood loss.
Children can sometimes have nosebleeds in their sleep. You can treat most nosebleeds at home, and you can take steps to help your child prevent them.
What causes nosebleeds?
The skin inside your child’s nose is very delicate. It's filled with many tiny blood vessels. That’s why even a small injury can bleed a lot. The most common causes of nosebleeds in children include:
-
Nose picking or frequent rubbing of the nose
-
Putting a foreign object in the nose
-
Dryness inside the nose
-
Allergies, colds, or other upper respiratory infections
-
Certain medicines
-
Injury to the nose
-
Abnormal tissue growths such as polyps
How are nosebleeds treated?
Nosebleeds are easy to treat at home. With correct treatment, most nosebleeds will stop in less than 5 to 10 minutes.
Based on the age of your child, the cause of their nose bleed, or both, the healthcare provider will tell you how to care for your child's nosebleed. Always call the provider to discuss your child's nosebleeds.
Keep the following list of dos and don’t s in mind.
DO
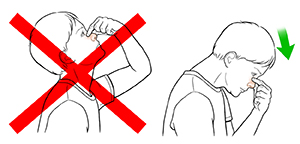 |
| Leaning back is the wrong way to stop a nosebleed. Instead, have your child lean forward and apply pressure to the nostrils. |
-
Keep your child calm and comfort them. Make sure they are breathing through their mouth normally.
-
Have your child sit or stand and lean their head forward (NOT backward). This keeps blood from pooling at the back of the throat, where it may be swallowed. If your child appears to be swallowing blood or has a lot of blood in the mouth, have them spit the blood out. If swallowed, it can lead to vomiting.
-
Ask older children to gently blow their nose. Then squeeze the lower third (soft part) of the nose with your thumb and forefinger. Younger children may not understand how to blow gently.
-
Continue squeezing the nose for 5 to 10 minutes without looking to see if bleeding has stopped.
-
If bleeding continues, repeat the step above by squeezing the nose for 5 to 10 minutes on the lower third of the nose without looking to see if bleeding has stopped.
-
You can also put a cold compress or ice pack to the "bony" bridge of the nose.
-
If the bleeding doesn't stop, contact your child's healthcare provider right away or go to the emergency room or urgent care clinic.
-
Once the bleeding stops and a clot forms, discourage rubbing or blowing the nose for several days. This will allow the blood vessels to heal.
-
Wash your hands carefully with soap and clean, running water after taking care of your child’s nosebleed.
-
Let your child sit down if they want, but don’t let them lie down during a nosebleed.
-
Your child may wish to take it easy for the rest of the day after a nosebleed.
-
Contact your child's healthcare provider before giving your child any over-the-counter medicine, especially for the first time.
DON’T
-
Don’t have your child lie down, tilt their head back, or place their head between their knees during the nosebleed. This is not needed, and may even make the nosebleed worse.
-
Don't put gauze or tissues in your child's nose to stop the bleeding.
-
Don’t give your child aspirin or ibuprofen.
-
Don't give your child a pain reliever. If your child needs one, call your healthcare provider.
-
Don't smoke or allow others to smoke in the home or around your child.
If nosebleeds happen often
If your child is having nosebleeds often, take them to see their healthcare provider or another provider who specializes in treating ears, noses, and throats (ENT). Your child may need a saline (special saltwater) nasal spray, nasal gel, or nasal ointment to moisten the inside of the nose, especially in the winter. Follow all instructions when using these on your child. In some cases, the healthcare provider may need to do a quick procedure to keep the vessels from bleeding.
How are nosebleeds prevented?
To help prevent nosebleeds in your child:
-
Use a nasal saline gel or nasal ointment to moisten the inside of the nose, especially in the winter. Use these products on the inside of your child’s nose before bedtime.
-
Try to keep your child from frequently rubbing their nose.
-
Try to keep your child from picking their nose. Nose picking is a common cause of nosebleeds. Keep their fingernails trimmed to reduce nose injury.
-
Treat nasal allergies. This may help stop cycles of itching, picking or scratching, and bleeding. Contact your child's healthcare provider before giving them any over-the-counter medicine, especially for the first time.
-
Use a vaporizer to add humidity to the air, if the provider advises it. Clean and dry the humidifier daily to prevent bacteria and mold growth. Don't use a hot water vaporizer. It can cause burns.
-
Avoid smoking and exposure to secondhand smoke.
When to call your child's healthcare provider
Call your child’s healthcare provider right away if your child has any of the following:
Call 911
Call 911 or seek emergency care right away for any of the following:
-
Trouble breathing or chest pain
-
Not acting normally
-
Crying or fussing that can't be soothed
-
Bruising on the abdomen, backs of thighs, or buttocks (these are fleshy places that don’t normally bruise)
-
Small, flat, purple spots (petechiae) anywhere on your child’s body
-
Pale skin or weakness anywhere in the body
-
Bleeding from a second area, such as the gums
-
Blood in the stool
-
Very heavy bleeding, with large clots visible
-
Bleeding that doesn't stop after 30 minutes of direct pressure or you can’t stop the bleeding
-
Multiple nosebleeds